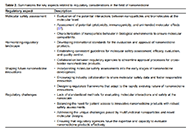
Focus on selecting high quality works
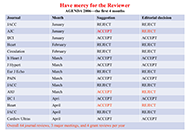
Transparent and reasonable process flow
Scientific rigour for every article
Waive APC in the first 5 years
Journals
Editors (Average H index 40+)
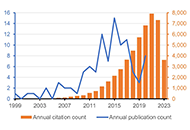
Articles
Views
Downloads


Prof. Jinwei Zhang
Published Articles: 11

Andrea Gomez-Zavaglia
Published Articles: 6

Prof. Reinhard Graf
Published Articles: 9

Prof. Ingrid Terreehorst
Published Articles: 6

Prof. Juergen Reichardt
Published Articles: 9

Prof. Karina Wierzbowska-Drabik
Published Articles: 6

Flexible Time Management and Status Control

Two-Way Matching for Efficient Peer Review

One-Stop Review Management

Points Reward and Quality Control