255 results in Exploration of Immunology
Latest
Sort by :
- Latest
- Most Viewed
- Most Downloaded
- Most Cited
Open Access
Review
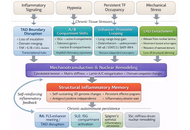
Epigenetic and metabolic reprogramming in autoimmune rheumatology: toward immune tolerance reprogramming
Ola A Al-Ewaidat, Moawiah M Naffaa
Published: May 29, 2026 Explor Immunol. 2026;6:1003255
Open Access
Review
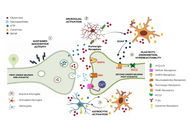
Is neuroinflammation the common thread in chronic pain? Recent advances and implications of the role of glial cells
Silvia Natoli ... Maurizio Marchesini
Published: May 27, 2026 Explor Immunol. 2026;6:1003254
This article belongs to the special issue Immunology and Pain
Open Access
Perspective
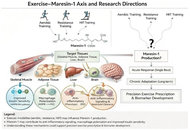
Does exercise enhance maresin-1 production? A new direction in metabolic anti-inflammatory research
Mehran Alipour ... Hassane Zouhal
Published: May 09, 2026 Explor Immunol. 2026;6:1003253
This article belongs to the special issue Physical Activity and Immune System in Chronic Diseases: Mechanisms and Insights
Open Access
Original Article
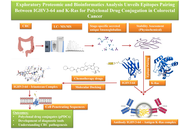
Exploratory proteomic and bioinformatics analysis unveils epitope pairing between IGHV3-64 and K-Ras for polyclonal drug conjugation in colorectal cancer
Raajesh Anand ... Ravikumar Sambandam
Published: May 07, 2026 Explor Immunol. 2026;6:1003252
Open Access
Review
Balancing analgesia and immunity: revisiting the immune consequences of opioid therapy
Lucia Daiana Voiculescu ... Sanjay Menghani
Published: April 28, 2026 Explor Immunol. 2026;6:1003251
This article belongs to the special issue Immunology and Pain
Open Access
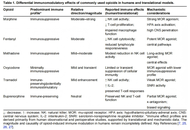
Original Article
C-reactive protein, procalcitonin, and neutrophil-to-lymphocyte ratio as mortality predictors in elderly women with pneumonia
Irawaty Djaharuddin ... Demak Lumban Tobing
Published: April 23, 2026 Explor Immunol. 2026;6:1003250
Open Access
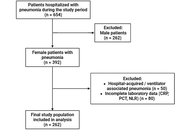
Original Article
Evaluation of the relationship between serum calprotectin and serum amyloid A with musculoskeletal ultrasonographic findings in rheumatoid arthritis patients
Noura Mohamed Abd El Maksoud Shehata ... Thanaa Farag Mansour
Published: April 20, 2026 Explor Immunol. 2026;6:1003249
Open Access
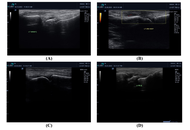
Protocol
Protocol workflow for whole blood memory B cell phenotyping and vaccine-specific antibody quantification
Jalilah Jamaluddin ... Intan Hakimah Ismail
Published: April 20, 2026 Explor Immunol. 2026;6:1003248
Open Access
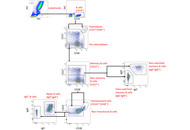
Review
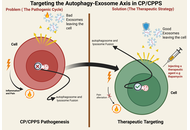
The autophagy-exosome axis in chronic prostatitis/chronic pelvic pain syndrome: a hypothesis-driven narrative review
Daniel Kofi Nyame ... Xiaohui Zhou
Published: April 16, 2026 Explor Immunol. 2026;6:1003247
Open Access
Review
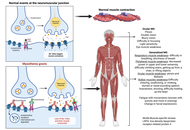
An update on cellular and molecular treatment of myasthenia gravis
Shaan Patel ... Vikrant Rai
Published: April 13, 2026 Explor Immunol. 2026;6:1003246
This article belongs to the special issue Advances in Cellular and Molecular Treatment of Autoimmune Diseases
Open Access
Review
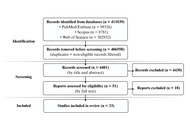
Variants in immune-related genes and their association with breast cancer risk and clinical behavior: an integrative review
Murilo Porfírio de Aguiar ... Jéssica Ferreira Vieira
Published: April 13, 2026 Explor Immunol. 2026;6:1003245
Open Access
Review
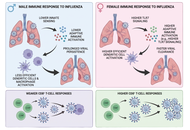
The influence of sex and gender differences in shaping the immune response to influenza infection and vaccination
Anna Calabrò ... Calogero Caruso
Published: April 13, 2026 Explor Immunol. 2026;6:1003244
Open Access
Review
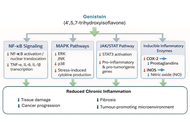
Genistein as a multi-target therapeutic: translational advances in inflammation and cancer
Satyajit Tripathy, Motlalepula Gilbert Matsabisa
Published: April 09, 2026 Explor Immunol. 2026;6:1003243
Open Access
Review
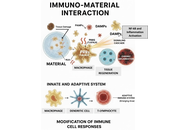
Immuno-materials: exploring the translational aspects among immunology, biomaterials and biomedicine
Marco Tatullo ... Francesco Paduano
Published: March 29, 2026 Explor Immunol. 2026;6:1003242
This article belongs to the special issue Immuno-Materials: at the interdisciplinary of immunology and materials
Open Access
Review
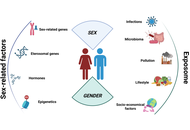
Autoimmune diseases are more common in women: insights into sex and gender differences in autoimmunity
Anna Calabrò ... Giuseppina Candore
Published: March 24, 2026 Explor Immunol. 2026;6:1003241
Open Access
Review
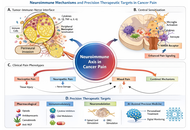
Cancer, immunity, and pain
Giustino Varrassi ... Matteo Luigi Giuseppe Leoni
Published: March 15, 2026 Explor Immunol. 2026;6:1003240
Open Access
Short Communication
Serum occludin as a novel biomarker in adult atopic dermatitis: a pilot case-control study
Sheron Tune Jawahar ... Kakithakara Vajravelu Leela
Published: March 11, 2026 Explor Immunol. 2026;6:1003239
Open Access
Review
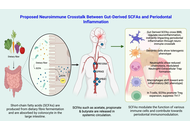
Immunomodulatory roles of gut-derived short-chain fatty acids in periodontal inflammation and homeostasis
Devlina Ghosh ... Damini Pandey
Published: March 11, 2026 Explor Immunol. 2026;6:1003238
Open Access
Review
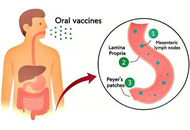
Postbiotics as promising oral vaccine adjuvants
Roya Abedi Soleimani ... Aziz Homayouni Rad
Published: February 13, 2026 Explor Immunol. 2026;6:1003237
Open Access
Review
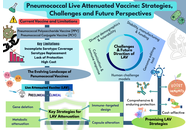
Pneumococcal live attenuated vaccine: strategies, challenges and future perspectives
Marina Yusoff ... Malik Amonov
Published: January 26, 2026 Explor Immunol. 2026;6:1003236
This article belongs to the special issue Novel Vaccines development for Emerging, Acute, and Re-emerging Infectious Diseases
 Previous
Previous