6 results in Exploration of Neuroprotective Therapy
Latest
Sort by :
- Latest
- Most Viewed
- Most Downloaded
- Most Cited
Open Access
Review
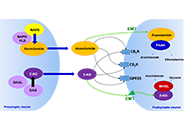
Therapeutic potential of the cannabinoid receptor 2 in neuropsychiatry
María S. García-Gutiérrez ... Jorge Manzanares
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:55–71
Open Access
Review
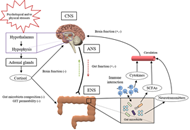
Gut microbial imbalance and neurodegenerative proteinopathies: from molecular mechanisms to prospects of clinical applications
Paula Alonso-García ... Eva Martínez-Pinilla
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:33–54
Open Access
Review
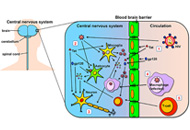
Neurological complications during HIV infection
Jose M. Martinez-Navio
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:19–32
Open Access
Review
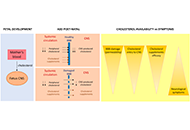
Cholesterol in autism spectrum disorders
Rafael Franco ... Irene Reyes-Resina
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:10–18
This article belongs to the special issue Cholesterol Dyshomeostasis in Neurological Diseases
Open Access
Letter to the Editor
P2X7 receptor involvement in COVID-19 disease
Peter Illes
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:7–9

Open Access
Editorial
Science plus technology to address challenges in determining the efficacy of neuroprotective/neurorestorative therapies
Rafael Franco
Published: August 05, 2021 Explor Neuroprot Ther. 2021;1:1–6

Journal Information