6 results in Exploration of Targeted Anti-tumor Therapy
Latest
Sort by :
- Latest
- Most Viewed
- Most Downloaded
- Most Cited
Open Access
Review
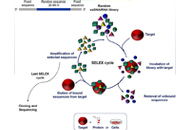
Aptamers and antibodies: rivals or allies in cancer targeted therapy?
Lisa Agnello ... Laura Cerchia
Published: February 28, 2021 Explor Target Antitumor Ther. 2021;2:107–121
Open Access
Review
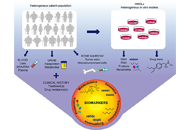
Multi-omics tumor profiling technologies to develop precision medicine in multiple myeloma
Sara Ovejero, Jerome Moreaux
Published: February 28, 2021 Explor Target Antitumor Ther. 2021;2:65–106
This article belongs to the special issue Off-Label Drugs and -Omics Data in Cancer Treatment
Open Access
Review
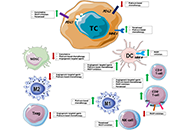
Immunotherapy in gynecological cancers
Domenica Lorusso ... Giovanni Scambia
Published: February 28, 2021 Explor Target Antitumor Ther. 2021;2:48–64
This article belongs to the special issue Immunotherapy in Cancer Patients

Open Access
Review
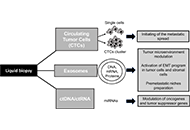
Non-invasive detection of epithelial mesenchymal transition phenotype and metastatic dissemination of lung cancer by liquid biopsy
Viviana De Rosa ... Francesca Iommelli
Published: February 28, 2021 Explor Target Antitumor Ther. 2021;2:36–47
This article belongs to the special issue Liquid Biopsy in Thoracic Cancer
Open Access
Review
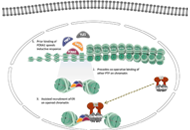
Emerging role of pioneer transcription factors in targeted ERα positive breast cancer
Honey Pavithran, Ranjith Kumavath
Published: February 28, 2021 Explor Target Antitumor Ther. 2021;2:26–35
This article belongs to the special issue Targeting Transcription Factors for Cancer Therapy
Open Access
Review
Old but gold: the role of drug combinations in improving response to immune check-point inhibitors in thoracic malignancies beyond NSCLC
Luca Cantini ... Rossana Berardi
Published: February 28, 2021 Explor Target Antitumor Ther. 2021;2:1–25
This article belongs to the special issue Immunotherapy in Cancer Patients