4 results in Exploration of Medicine
Latest
Sort by :
- Latest
- Most Viewed
- Most Downloaded
- Most Cited
Open Access
Review
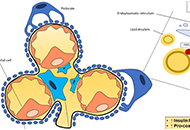
PNPLA3 gene and kidney disease
Alessandro Mantovani, Chiara Zusi
Published: February 29, 2020 Explor Med. 2020;1:42–50
Open Access
Original Article
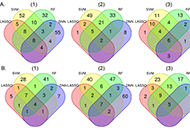
Identifying factors associated with opioid cessation in a biracial sample using machine learning
Jiayi W. Cox ... Lindsay A. Farrer
Published: February 29, 2020 Explor Med. 2020;1:27–41
This article belongs to the special issue The Biological Basis of Substance Use Disorders
Open Access
Review
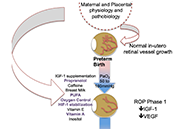
Current evidence and outcomes for retinopathy of prematurity prevention: insight into novel maternal and placental contributions
Lara Carroll, Leah A. Owen
Published: February 29, 2020 Explor Med. 2020;1:4–26
Open Access
Editorial
Welcome message from the Editor-in-Chief
Lindsay A. Farrer
Published: February 29, 2020 Explor Med. 2020;1:1–3
