Affiliation:
1Department of Hotel and Restaurant Business Management, State University of Trade and Economics, 02156 Kyiv, Ukraine
Email: l.bovsh@knute.edu.ua
ORCID: https://orcid.org/0000-0001-6044-3004
Affiliation:
1Department of Hotel and Restaurant Business Management, State University of Trade and Economics, 02156 Kyiv, Ukraine
ORCID: https://orcid.org/0000-0002-0498-3433
Affiliation:
2Department of Management, State University of Trade and Economics, 02156 Kyiv, Ukraine
ORCID: https://orcid.org/0000-0001-7380-5000
Explor Digit Health Technol. 2026;4:101189 DOI: https://doi.org/10.37349/edht.2026.101189
Received: November 24, 2025 Accepted: February 09, 2026 Published: March 11, 2026
Academic Editor: Andy Wai Kan Yeung, The University of Hong Kong, China
Aim: The aim of this study is to analyse the digital patient journey in medical tourism, with a particular focus on Ukraine’s experience under conditions of military challenges and global crises. The study examines how digital tools support inclusivity, accessibility, continuity of care, and patient trust, with special attention to rehabilitation services and vulnerable patient groups affected by war.
Methods: The study employs a mixed-methods approach combining a review of scientific literature with empirical research and modelling of the digital patient journey. Primary data were collected through an online survey of 150 healthcare consumers and semi-structured interviews with 15 experts representing medical institutions involved in medical tourism. Quantitative and qualitative analyses were used to examine patient experience, inclusivity barriers, and the role of digital services.
Results: The results indicate that key stages of the digital patient journey include online information search and clinic selection, remote consultations, digital support for travel and treatment organization, and post-treatment follow-up and rehabilitation. Ukrainian clinics actively implement CRM systems, telemedicine solutions, and digital communication tools, enabling continuous patient engagement even during crisis conditions. At the same time, significant barriers were identified, including limited inclusiveness of digital services, data security concerns, uneven digital literacy, and infrastructural constraints. Based on the findings, a conceptual model of the digital patient journey integrating service quality, inclusivity, and AI-supported personalization was developed.
Conclusions: The findings demonstrate that the digital patient journey is becoming critically important for the development of medical tourism under conditions of global uncertainty. The integration of digital tools with inclusive and patient-centred approaches enhances the resilience of medical services, strengthens patient trust, and provides competitive advantages for medical institutions. The proposed model may be useful for countries experiencing military conflicts or systemic crises and contributes to the broader development of digital and inclusive healthcare.
The COVID-19 pandemic has been a catalyst for big changes in international healthcare system. It highlights the need for strategic implementation of digital solutions that can ensure continuity of medical services, data protection and equitable access for diverse groups of users. In response to these challenges, the World Health Organization (WHO) has developed the Global Strategy on Digital Health 2020–2025, which defines key areas for integrating technology into medical practice [1]. These strategic guidelines are consistent with UN Sustainable Development Goals, in particular SDG3 “Good health and well-being” and SDG10 “Reduced inequalities” [2]. This highlights the role of digital innovation as a tool for achieving equity, inclusion and sustainability on a global scale. At the same time, the need for rehabilitation and inclusion medical services remains one of the most unsolved healthcare issues. The WHO Rehabilitation 2030 initiative [3] focuses on the widespread inadequacy of rehabilitation services and the need to integrate them into national healthcare system as a part of universal coverage.
Therefore, the digital transformation of the medical sector is radically changing the way patients search for, select, and receive medical services, as well as interact with service suppliers in international medical tourism communication. Recent bibliometric and systematic research reviews on this topic highlights rapid growth of scientific interests in the digital optimization of the patient journey in medical tourism, with a focus on the role of telemedicine, mobile applications, online registration systems, and data analysis tool for personalizing services [4, 5].
In addition, the intensification of regional and global crises, including military conflicts, terrorist attacks, and pandemics, is driving demand for models that combine digital solutions with inclusive support approaches for vulnerable groups (the wounded, people with disabilities, displaces persons), which requires specialized methods of interface adaptation, language support, and rehabilitation digital services [5, 6].
Despite the general revival of research in the field of digital medical tourism, there are gaps in the literature regarding the integrated consideration of the digital patient journey, taking into account rehabilitation needs and inclusion in the context of crisis or post-conflict countries. Precious studies by the authors have already shown that digital marketing strategies, Customer Relationship Management (CRM) systems, and telehealth tools increase patient engagement and the competitiveness of medical tourism providers [7]. Further analysis of digital solutions in the field of rehabilitation services revealed the need to adapt them to inclusive design and the specifics of working with vulnerable groups, in particular those affected by war [8]. This study is a logical continuation of previous work and aims to combine the perspective of the digital patient journey with an emphasis on inclusion and rehabilitation in the context of global challenges.
Key terms used in this study, such as medical tourism (MT) and digital medical tourism (DMT), are defined in the Supplementary material.
A combined approach was employed in the study due to its research nature and the need for an in-depth understanding of digital transformation processes in the medical field. The main goal is to identify and analyze key elements of the digital patient journey in medical tourism, with a particular focus on Ukraine’s experience as an example of adaptation to military challenges and global crises.
The methodological basis was provided by empirical research and case study, which make it possible to identify best practices in digital communication with patients at different stages of their medical journey. To collect primary data, an online survey was conducted among respondents who had sought treatment or rehabilitation services at Ukrainian or foreign clinics, including war victims and persons with disabilities. The survey included questions about their reasons for seeking treatment, expectations, satisfaction with digital services (telemedicine, mobile apps, chatbots, CRM systems), and barriers to accessing inclusive solutions.
In addition, comparative and content analysis of WHO strategic documents were used, as well as specialized analytics on digital health practices. This made it possible to correlate the survey results with global trends and identify potential areas for adapting digital technologies in field of medical tourism. The use of case study made it possible to conduct a more in-depth analysis of the experience of specific Ukrainian clinics that implemented digital solutions under crisis conditions and to evaluate their effectiveness from the perspective of patient experience.
The research methodology is based on data analysis and consists of certain stages. First, basic hypotheses were formulated concerning the impact of digital solutions on patient satisfaction, barriers to inclusion, willingness to choose the clinic again, and adaptation of international practices. Then, the theoretical basis for substantiating the was developed. The theory of brand as a social construct and empirical models of the patient journey (Table 1) formed the scientific basis.
The relationship between hypotheses, methods, and theoretical foundations.
| Hypotheses | Research methods | Analysis | Theoretical foundations |
|---|---|---|---|
| H1: Patients who have access to modern digital tools rate their medical tourism experience much higher | Online surveys (use of mobile applications, telemedicine, chatbots) | Descriptive statistics, comparison of user/non-user groups | Diffusion of Innovations |
| H2: Insufficient inclusiveness and accessibility of digital services are key barriers for patients with disabilities and victims of war | Surveys (access barriers), expert interviews | Sample segmentation (veterans, people with disabilities, civilians), qualitative comparison | Inclusive Design Framework, Social Model of Disability |
| H3: The high level of digitalization in clinics (telemedicine, mobile applications, online support) has a positive impact on patients’ willingness to choose the clinic again | Surveys (criteria for deciding whether to reapply), expert interview | Correlation between level of digitalization and “intention to return” | SERVQUAL model, CRM theory |
| H4: Ukrainian patients see potential for the development of digital medical tourism based on international practices, especially in the rehabilitation and inclusion segment | Comparative analysis with survey, modeling | Comparing patients’ expectations with global practices | Resource-Based View (RBV) |
The next step was to obtain primary data on consumers’ experience in communication with clinics and medical tourism entities. To this purpose, an empirical survey-based study was conducted. The structured questionnaire included sections on reasons for seeking treatment, use of digital services, satisfaction, access barriers, and expectations regarding inclusive medicine.
The survey was distributed to a total of 200 potential respondents via multiple channels to ensure broad reach: 120 invitations through social networks (Facebook, LinkedIn, Telegram) and 80 invitations via partner clinics and medical institutions in Kyiv and other regions. Out of these, 150 respondents completed the survey, resulting in a 75% completion rate. The average time to complete the survey was 8 minutes, with the highest attrition observed in sections containing open-ended questions (approximately 10%). Data collection took place between 15 September and 15 November 2025.
The sample consisted of patients of Ukrainian clinics, including foreign medical tourists, with particular emphasis on war victims and persons with disabilities, to assess the inclusiveness of digital solutions. Additional expert interviews were conducted with clinic representatives to complement survey data. All responses were collected via Google Forms without storing personal identifiers, ensuring anonymity and ethical compliance. Aggregated data, including completion rates, time to completion, and attrition, are presented in the article to improve methodological transparency and are available upon request.
The next stage involved data processing and analysis. To test the hypotheses and compare the results with global trends, descriptive statistics, comparative analysis of responses from different patient groups, and content analysis of international strategies (WHO Global Strategy on Digital Health 2020–2025, Rehabilitation 2030, SDGs) were used.
The final stage of study was a qualitative verification of the hypotheses put forward, which was carried out by comparing the quantitative results obtained with practical cases of digitalization in the field of medical tourism. For this purpose, a qualitative analysis of best practices was used, which made it possible to identify innovative formats of interaction between clinics and patients. In addition, scenarios for integrating digital services into the patient journey were modeled, and possible partnership models (joint investments, technological collaborations, digital franchising). This approach made it possible to interpret potential market development trajectories and identify the balance of benefits and risks for Ukrainian medical institutions in the context of military challenges and global instability.
The study is part of a larger research project on crisis management for medical tourism entities and aims to provide a scientific basis for the development of partnership models in the field of digital medicine.
Today, the use of digital tools and interaction on digital platforms is the norm in consumer-business relations. However, consumer behavior in the field of medical tourism is determined not only by the quality of services provided, but also by a complex of socio-demographic and cultural patterns: age, gender, country of residence, level of digital skills, expectations, and motivation for seeking treatment. These variables shape different scenarios for the perception of the medical experience, particularly in the context of digital interaction between the patient and the clinic. To understand the specifics of the digital patient journey in the Ukrainian context, it is important to outline the social profile of respondents who participated in the study and identify the key trends that influence their assessment of service (Table 2).
Survey participant profiles.
| Indicator | Category | Quantity | % |
|---|---|---|---|
| Age | ≤ 25 years old | 36 | 24.0 |
| 26–35 years old | 43 | 28.7 | |
| 36–45 years old | 38 | 25.3 | |
| 46–55 years old | 24 | 16.0 | |
| ≥ 56 years old | 9 | 6.0 | |
| Gender | female | 124 | 82.7 |
| male | 21 | 14.0 | |
| other | 5 | 3.3 | |
| Country of residence | Ukraine | 144 | 96.0 |
| others | 6 | 4.0 | |
| Health status/Special needs | war victims | 39 | 26.0 |
| disability | 14 | 9.3 | |
| other | 97 | 64.7 | |
| Experience in medical tourism | yes | 49 | 32.7 |
| no | 101 | 67.3 | |
| Experience with digital services | actively use (online registration, telemedicine, mobile apps, etc.) | 85 | 56.7 |
| partially | 45 | 30.0 | |
| do not use | 20 | 13.3 |
Source: developed by the authors.
The impetus of the study was the cumulative impact of insurmountable crisis factors: the COVID-19 pandemic and full-scale war in Ukraine have triggered the need for safe, remote, and flexible formats for obtaining medical services, particularly in the field of medical tourism. The coronavirus pandemic has created a global digital shift in the “patient-medical facility” communication model. Patients in Ukraine and around the world have increasingly adopted telemedicine, online booking and registration, and mobile health applications for monitoring their health. This contributed to the formation of expectations of “instant access” to consultations, personalized solutions, and convenience regardless of location. It was during this period that the practice of remote medical trust became established—when the patient chose a clinic based not so much on the offline reputation of the doctor as on their digital presence, ratings, and reviews on social media. The full-scale war, in turn, has created a new type of patient- one who is traumatized, mobile, pragmatic, and at the same time vulnerable. For many Ukrainians, medical tourism has become not just a choice, but also a forced strategy for seeking safety, treatment, or rehabilitation. The proposition of the patients with disabilities injures and post-traumatic stress disorder is growing. This request not only includes physical accessibility, but also inclusive digital services: adapted interfaces, online follow-up, translation, and psychological supports.
In managing communications in the field of medical tourism, the key players are specialists from medical institutions and travel companies who are directly involved in shaping the medical tourism product. An important step is therefore to evaluate the effectiveness of the digital patient journey by experts in the medical field, who were also interviewed during the study. The sample include 15 respondents working in the field of digital and traditional medicine: department heads (5 people); doctors (1 rehabilitation specialist, 1 surgeon, 1 oncologist, 1 psychologist); managers/specialists in medical tourism and communications (2 medical tourism managers, 1 telemedicine expert, 1 clinic communication manager, 1 digital product manager, 1 international manager flow manager) (Table 3).
Profiles of participants in semi-structured interviews.
| Variables | Elements | Frequency | % |
|---|---|---|---|
| Position | Department heads in medical institutions | 5 | 33.3 |
| Doctors | 4 | 26.7 | |
| managers/specialists in medical tourism and communications | 6 | 40.0 | |
| Experience in the field of healthcare | 2–5 years | 0 | 0.0 |
| 6–8 years | 4 | 26.7 | |
| 9–12 years | 6 | 40.0 | |
| 13–15 years | 5 | 33.3 | |
| Region | Kyiv | 10 | 66.7 |
| Kharkiv | 2 | 13.3 | |
| Lviv | 2 | 13.3 | |
| Odesa | 1 | 6.7 |
Source: developed by the authors.
The selection was made using purposive sampling, taking into account the relevant experience of respondents (at least 2 years of work in the field of medical tourism).
So, expert respondents have an average of 11 years of experience, which makes them qualified to assess digital services and patient experience. Moreover, the regional coverage (Kyiv, Kharkiv, Lviv, Odesa) makes it representative of the Ukrainian medical tourism expert.
Recent scientific literature on healthcare [4, 9–12] notes the formation of a new paradigm—Digital Patient Experience (DPE), which covers the entire patient journey: from initial search for information, choice of medical facility, online registration, treatment/rehabilitation, to post-treatment follow-up. This experience is no longer limited to the quality of medical care in the doctor’s office—it includes the quality of digital interaction, level of transparency, convenience, responsiveness, and emotional support.
Let’s explore the experience of digital medical tourism in Ukraine, which is known for its affordable and high-quality medical services, before the full-scale war. After all, in conditions of increasing physical risk to patients, where factors such as war, internal displacement, and limited access to medical infrastructure combine, the importance of telemedicine, online consultations, and inclusive digital services as key elements of safe and effective patient experience is growing.
Respondents involved in obtaining information about medical services use various sources (Figure 1).
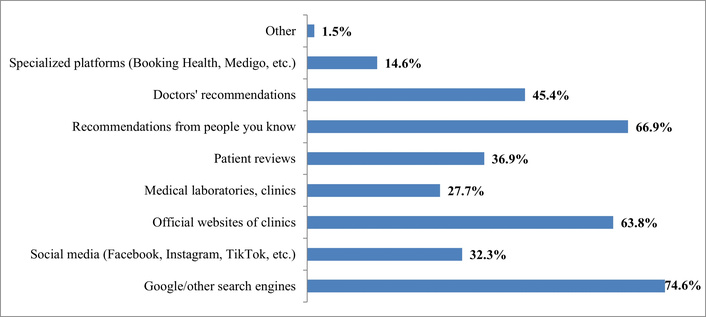
Interpretation of answers to the question “Where do you usually look for information about medical services? (Multiple options can be selected)”. Source: compiled from anonymized survey results.
Therefore, the experience of Ukrainian patients covered both traditional (recommendations from acquaintances—66.9%) and digital channels (search internet systems—74.6%, official clinic websites—63.8%).
At the same time, it is important to assess the level of use of digital services in Ukrainian patients (Figure 2).
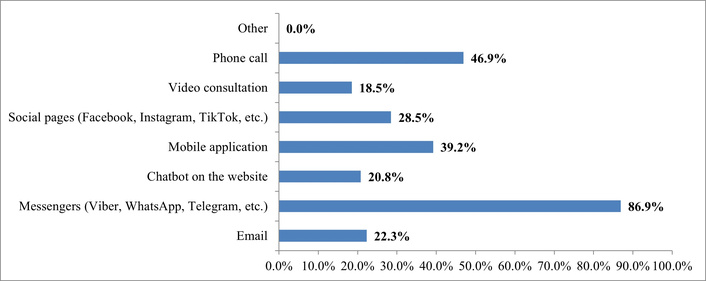
Interpretation of answers to the question “What digital communication channels are most convenient for you? (Multiple options can be selected)”. Source: compiled from anonymized survey results.
The results of a survey on the convenience of digital communication channels showed that messengers (Viber, WhatsApp, Telegram, etc.) are the most popular among patients, with 86.9% of respondents choosing them. This indicates the preference for fast, intuitive, and personalized interaction formats that correspond to the modern style of digital user behavior. Telephone call ranks second (46.9%), remaining relevant due to the trust placed in direct voice contact with a medical representative.
At the same time, mobile applications (39.2%) and social networks (28.5%) demonstrate the growing role of multi-channel presence of medical organizations in the digital space. Chatbots on websites (20.8%) and video consultations (18.5%) remain less popular, which may be explained by limited user experience or distrust of automated services.
Let’s explore this issue through the respondents’ answers. The results are shown in Figure 3.
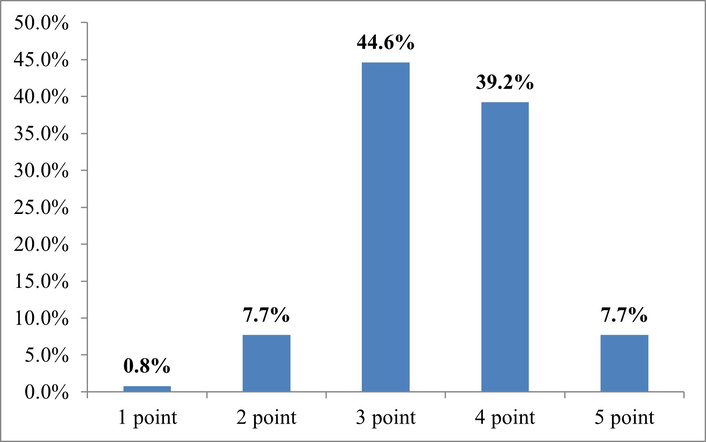
Interpretation of answers to the question “How much do you trust digital health services compared to traditional consultations? Rate on a scale of 1–5 (1—I don’t trust at all, 5—I trust completely)”. Source: compiled from anonymized survey results.
Trust in digital medical services in Ukraine is moderate, reflecting the gradual adoption of the digital patient journey. According to the survey results, most respondents rated their level of trust at 3 (44.6%) or 4 points (39.2%), indicating a positive but not yet stable perception of digital medical tools. Only 7.7% of respondents express a high level of trust (5 points), while 8.5%—minimal level (1–2 points). These results show that patients who already have experience with online consultations generally rate digital services as useful and convenient, but need greater confidence in their security, personalization, and quality of feedback. The benefits of choosing communication channels are further proof of the growth in digital trust. Messengers (Viber, WhatsApp, Telegram тощо) have become the most convenient communication channel for 86.9% of respondents. This reflects patients’ desire for fast, informal, and personalized communication with medical institutions. Phone calls remain relevant for 46.9% of respondents, while mobile apps (39.2%) and clinics’ social media pages (28.5%) serve as additional channels of engagement. Less common are chatbots on websites (20.8%) and video consultations (18.5%), indicating a need to improve the quality of digital interaction and technical support for users.
The consistency of respondents’ answers is confirmed by the fact that 63.8% of those surveyed already have experience with online consultations, indicating the gradual formation of a new norm of interaction between patients and clinics. At the same time, online consultations with a doctor (73.8%) and electronic health records and access to medical history (64.6%) are considered by patients to be key elements of a positive digital experience, contributing to convenience, time savings, and a sense of security when receiving medical services (Figure 4).
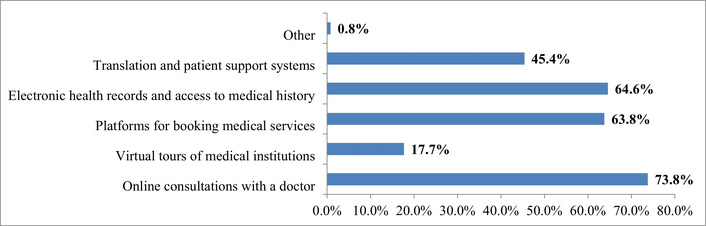
Interpretation of answers to the question “What digital services do you consider most important for medical tourism? (Multiple options can be selected)”. Source: compiled from anonymized survey results.
This result confirms that the digital patient journey is transforming from an additional option into a core component of medical services, shaping the level of patients’ satisfaction and trust. In particular, on the satisfaction scale, the vast majority of respondents rate their experience positively (Figure 5).
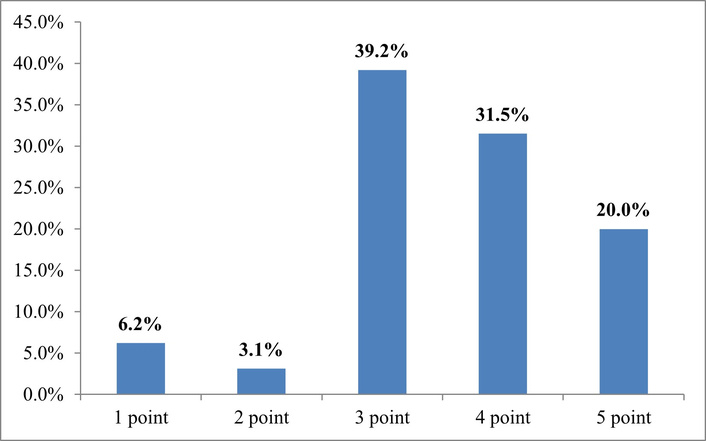
Interpretation of answers to the question “Rate your experience using online consultations on a scale of 1–5 (1—very dissatisfied, 5—very satisfied)” (on a Likert scale). Source: compiled from anonymized survey results.
This indicates that patients are moderately optimistic about the use of digital tools, but they are not yet fully confident in their reliability. This situation is due to both varying levels of digital literacy and the influence of external stress factors—the COVID-19 pandemic and the war, which have changed perceptions of the safety and quality of medical services.
Overall, online communication not only ensures the promptness and accessibility of medical care but also creates a sense of psychological security, which is especially important in conditions of increased stress, caused by war and forced migration. It is increasingly perceived as a sign of the quality and modernity of a clinic.
At the same time, the results of semi-structured interviews also demonstrate the focus of medical services on digital patient care (Table 4).
Interpretation of expert respondents’ answers in the context of their professional vision of which elements of Human-Centered Design are key for a digital tourism product.
| Digital medical service | Users need to be taken into account by digital services | Share of similar interpretations in respondents’ answers, % | Quote from interview |
|---|---|---|---|
| Mobile app for appointments and online consultations | Response speed, awareness, and remote access | 85.0% | “Patients who use our mobile app are almost always satisfied with the response speed and awareness”—clinic manager, Kyiv |
| Social media/online reviews | Information support, trust in the clinic, assistance in decision-making | 65.0% | “Younger patients and their relatives often choose a clinic after reviews on social media”—head of the rehabilitation department, Lviv |
| Telemedicine (video consultations) | Accessibility for people with disabilities, autonomy, and control over treatment | 75.0% | “The accessibility of telemedicine for patients with disabilities greatly influences their assessment of the service”—Expert in inclusive medicine, Kharkiv |
| Messengers (Viber, WhatsApp, Telegram) | Prompt communication, appointment reminders, and quick responses to questions | 80.0% | “Patients appreciate instant responses via messengers, which allows them quickly resolve issues without making phone calls”—clinic manager, Kyiv |
| Online registration for an appointment via the website | Convenient planning, time savings, and avoiding queues | 70.0% | “Online registration allows patients to choose a convenient time and avoid queues”—communication manager, Odesa |
| Chatbot on the website | Information support without waiting for an operator, answers to frequently asked questions | 60.0% | “The chatbot helps you get quick answers to standard questions without waiting for an operator”—clinic’s digital product manager, Lviv |
| Mobile app with personalized reminders | Treatment monitoring, personalized recommendations, increased sense of security | 70.0% | “Patients receive reminders about tests and doctors’ recommendations, which increases their confidence in the treatment process”—head of the patient experience department, Kyiv |
Source: developed by the authors.
Interviews with medical tourism experts confirm that modern digital services in clinics are focused on patient needs and increase patient satisfaction. Mobile applications and online consultations provide quick access to information and remote service, which is especially important for patients with disabilities and foreign tourists. Social networks and reviews help build trust and make it easier to decide on a clinic. Messengers and chatbots provide prompt communication and appointment reminders, increasing patient convenience and autonomy.
Therefore, digital services not only optimize international processes in clinics but also serve as a tool for patient care, creating a positive experience and increasing trust in medical services. They are a key element of a people-oriented approach in modern medical tourism. The digital patient journey represents a synergy of technological efficiency and an empathetic approach, in which service quality is determined not only by medical outcomes but also by the level of support, understanding, and convenience perceived by patients during remote interactions with clinics.
Overall, the empirical study formed an analytical basis for patient behavior patterns in modern conditions. Analysis of survey data and interviews with experts showed that access to modern digital services significantly affects the assessment of patient experience. Patients who actively use online appointments, mobile apps, and telemedicine consultations rate their experience significantly higher than those who limit themselves to traditional channels.
In this way, the digital patient journey enhances patient comfort, awareness, and control over their own health, forming the basis for a positive patient experience. It contributes to an increased subjective sense of security, convenience, and control over the treatment process, as well as strengthening patient trust in the medical brand.
So, the hypothesis that patients who have access to modern digital tools rate their medical tourism experience significantly higher is confirmed both by a review of scientific sources and by the results of empirical studies. This confirms the strategic importance of developing digital patient experience systems for international medical tourism.
In creating a positive patient experience issue of inclusivity and accessibility of digital services is important in today’s Ukrainian and global realities. Its theoretical basis is formed at the intersection of several theories. In particular, the Inclusive Design Framework guides the creation of digital products that take into account the needs of the widest possible range of users, regardless of their physical, cognitive, or social characteristics. It moves away from the “adaptation for minorities” approach and instead proposes universal design as a principle of equitable access. As noted by Coleman et al. [13] and Pullin and Higginbotham [14], inclusivity is not just a technical aspect—it is a philosophy of creating services that support the dignity, autonomy, and equal opportunities of the user. At the same time, the theory is complemented by research by Li et al. [15], who argue that the effectiveness of medical services can be improved by AI capabilities that can provide intelligent interventions to assist caregivers and patients.
These findings are confirmed by the results of interviews with medical experts (Table 5).
Interpretation of Inclusive Design Framework approaches based on interviews with expert respondents from the medical tourism industry.
| Inclusive Design Framework component | Analytical category (based on interview) | Typical respondent quotes | Interpretation for digital medical tourism |
|---|---|---|---|
| User diversity | Recognition of different physical and psychological conditions of patients (in particular, military persons, internally displaced, and persons with disabilities) | “Our online platforms should be accessible to both young and older people with visual or hearing impairments.” | The need to create adaptive interfaces and multi-format content (audio, subtitles, simplified text). |
| Equity | Expanding barrier-free access to online consultations, telemedicine, and support chats | “After the war began, we simplified registration and added a free online consultation feature for veterans.” | Inclusion as an element of social responsibility for clinics builds trust in the brand. |
| Flexibility in use | Multi-platform solutions (chatbots, mobile apps, video consultations) | “Patients choose the format themselves—chat, call, or video. This increases satisfaction and reduces the number of refusals.” | Digital flexibility as a factor in increasing accessibility and loyalty. |
| Cognitive accessibility | Reducing information overload, simplifying the interface | “Patients should not get lost in medical terminology. We test messages for clarity.” | Communication simplicity is the key to expanding the inclusiveness of the service. |
| Human–AI collaboration | Using algorithms for personalized care, detecting warning signs, and supporting caregivers | “The results of human-AI collaboration can provide smart intervention to help caregivers and patients, especially in rehabilitation.” | Intelligent systems support personalized сare, provide safe digital interventions, and monitor patient status. |
Source: developed by the authors.
The interview results show that Ukrainian clinics are gradually integrating inclusive design principles, but those institutions that combine the human factor with the technological empathy of AI achieve the best results. Such practices create a “smart care”, effect that is becoming a marker of trust in digital medical tourism.
The issue of inclusion is particularly relevant in the context of the war in Ukraine, where the number of people with injuries, post-traumatic conditions, and temporary mobility limitations has increased significantly. As recent studies show [1, 16, 17], war victims often have limited access to quality digital health services due to internet problems, a lack of adapted platforms, and low levels of digital literacy. In this way, inclusive digital design becomes not only a technological challenge but also a moral and social imperative in post-war medical reconstruction.
Based on this, in the second part of the study, we will examine the extent to which Ukrainian patients, particularly those with disabilities or who have suffered from the war, feel included in the digital medical environment and what barriers remain most significant in the use of digital health services.
The theoretical basis for this paradigm is the Social Model of Disability, which treats limitations not as a personal problem of the individual but as the result of barriers in the environment, particularly the digital environment. According to Shakespeare [18], it is social infrastructural and communication barriers that create disability in society. In the context of digital medicine, this means that inaccessible interfaces, the lack of alternative information formats, and low platform adaptability become factors in the digital alienation of patients [6].
The importance of barrier-free communication is confirmed by the results of a survey (Figure 6).
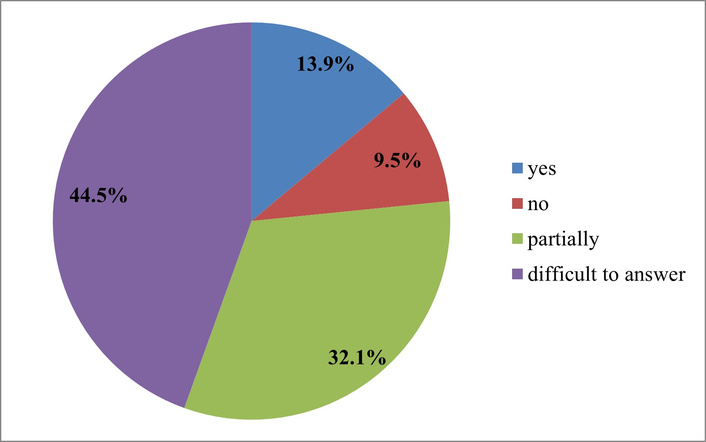
Interpretation of answers to the question “In your opinion, are the needs of people with disabilities sufficiently taken into account in digital medical services?”. Source: compiled from anonymized survey results.
The results obtained regarding the assessment of the extent to which digital health services take into account the needs of people with disabilities demonstrate a general feeling of a lack of inclusiveness of such solutions. Only 13.9% of respondents answered affirmatively, which indicates a low level of perception of digital services as fully accessible and adapted for users with disabilities.
Of particular note is the high proportion of “Difficult to answer” responses (44.5%), which is a critical indicator. Such uncertainty may be related not only to the lack of personal experience of interacting with inclusive digital solutions, but also to low transparency, insufficient communication between developers and health institutions about accessible options, or to the general limitation of inclusive functions in existing systems.
At the same time, 32.1% of the answers “Partially” indicate that users recognize some positive elements of inclusion, but they do not form a sufficient level of satisfaction or a feeling of full consideration of the needs of people with disabilities.
Thus, the survey results indicate that the development of digital medicine in Ukraine should include not only technological improvements but also a systematic focus on inclusive design, more transparent communication of available opportunities, and increasing user trust and autonomy. The combination of a low share of fully satisfied users and a significant share of those who could not give an unambiguous answer confirms the existence of gaps in the field of digital accessibility and the need for targeted inclusive policies.
Language barriers are also an important aspect of communication with clinics, particularly in international medical tourism, as evidenced by the results of a survey (Figure 7).
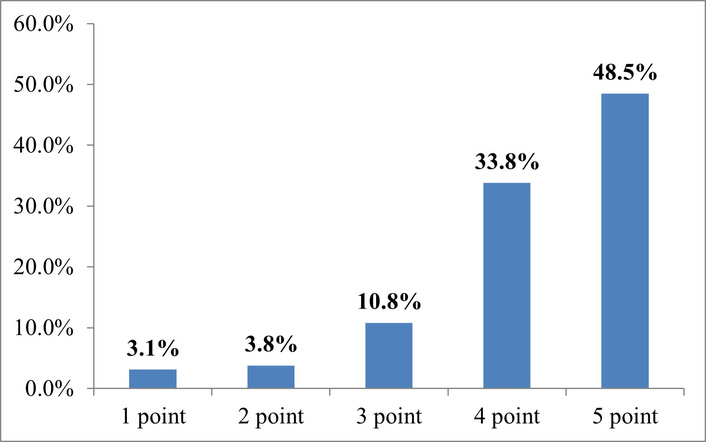
Interpretation of answers to the question “How important is translation and language support in digital medical tourism services to you?” (on a Likert scale). Source: compiled from anonymized survey results.
The growing role of post-treatment digital support as an element of trust and long-term interaction between patients and medical institutions is evidenced by the responses of consumers of medical services (Figure 8).
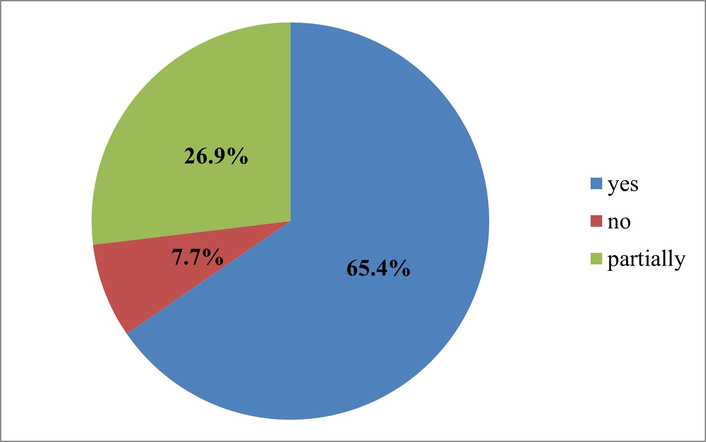
Interpretation of answers to the question “Is continued online support from a doctor important to you after returning home?”. Source: compiled from anonymized survey results.
At the same time, respondents prefer digital formats for support (Figure 9).
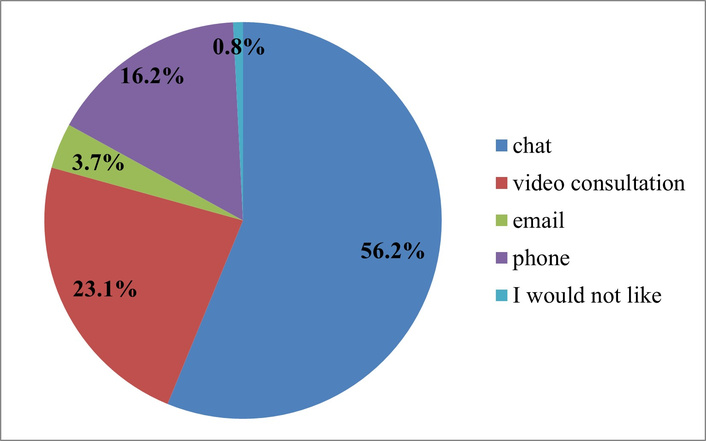
Interpretation of answers to the question “In what format would you like to receive further support?”. Source: compiled from anonymized survey results.
The results show that most patients (56.2%) prefer chat as the main format for follow-up support after treatment, which highlights the need for fast, convenient, and asynchronous communication. The results show that most patients (23.1%) prefer chat. On the other hand, telephone support (16.2%) and email (3.7%) are less popular, and only 0.8% of respondents do not need further communication. This confirms the trend toward digital interactivity and continuous patient support during rehabilitation. Therefore, patients expect not only high-quality treatment from clinic, but also convenient digital interaction after receiving services, where the main criteria are speed, personalization, and ease of use of communication channels.
The results confirm that the inclusiveness of digital medical services in Ukraine remains a partially implemented area that requires systematic support from both government policies and clinics themselves. Although there has been progress in the technological flexibility of services, barriers to inclusive access remain significant. According to the survey:
technical limitations (unstable internet connection, lack of adapted interfaces for people with visual or hearing impairments);
organizational barriers (low level of staff training in working with vulnerable patient groups in a digital environment);
socio-psychological factors, including distrust of online medical services, fear of using technology, digital literacy, or post-traumatic disorders in patients affected by war.
Together, these factors create digital inequality among patients, which affects not only the quality of medical care but also their level of social inclusion. That is why the Inclusive Care Model, which combines the principles of universal design, empathetic communication, and support algorithms based on AI technologies, should guide the development of digital medicine in Ukraine.
In the context of the trends discussed, it is important to consider key aspects of building long-term loyalty and digital competitive advantages in medical tourism. A patient’s decision to return to a clinic increasingly depends on the quality of their digital interaction with the medical institutions. The theoretical basis for analyzing this process is provided by the SERVQUAL model proposed by Parasuraman et al. [19], which defines service quality through the gap between expectations and actual perception of the service. According to the model, the key dimensions are reliability, responsiveness, assurance, empathy, and tangibles. In the study, Zimeras [20] presents an improved spatial SERVQUAL model in the healthcare system. In a digital environment, these parameters take on new dimensions, such as the availability of digital channels, uninterrupted online support, personalization of recommendations, and trust [10, 21–23].
Let us explore these issues in the Ukrainian context of medical services. First, let us find out how experts assess the level of digitalization of clinics and its impact on patients’ willingness to return. Therefore, the following questions were asked: 1) the number and quality of patient visits through digital channels (mobile applications, online registration, and telemedicine); 2) the frequency of repeat visits and patient loyalty; 3) the convenience of digital channels for patients; 4) problems and barriers in the use of digital services.
The integration of the responses is presented in Table 6.
Synthesis of the results of interviews with medical tourism experts on the level of digitalization of clinics and its impact on patients’ willingness to return and receive services.
| Parameter | Expert assessment | Typical comments/Issues |
|---|---|---|
| Number of inquiries via digital channels | High | Patients actively use mobile applications and online registration. Online registrations have increased by about 30–40% over the past year. |
| Quality of inquiries/patient awareness | Medium–high | Online patients are better prepared and ask specific questions. Some users do not fill out their medical history, which complicates the doctor’s work. |
| Repeated contacts/loyalty | High | Patients who use digital services are more likely to return (40–50% repeat visits). |
| Convenience of digital channels | High | Patients appreciate quick appointments, reminders, and telemedicine consultations. |
| Problems and barriers | Low–medium | Key problems: technical application failures, insufficient message personalization, and lack of integration with electronic medical records. |
Source: developed by the authors.
At the same time, potential patients base their choice of clinic on the following criteria (Figure 10).
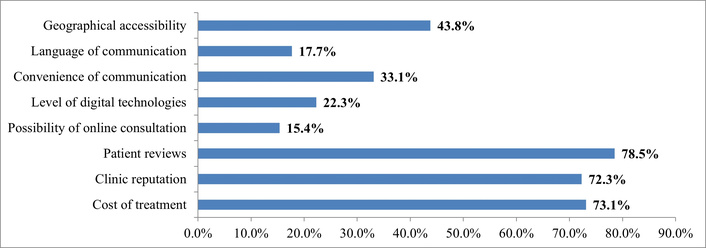
Interpretation of answers to the question “What factors most influence the choice of clinic? (Maximum 3 options)”. Source: compiled from anonymized survey results.
An analysis of responses from consumers of medical services showed that patient reviews play a primary role in choosing a clinic (78.5% of total responses), so it is important to establish quality feedback on the clinic’s website and social media pages. The second most important criterion in the decision-making process for consumers of medical services is the cost of treatment (73.1% of total responses). Third—the clinic’s reputation (72.3% of total responses), which indicates the importance of the quality of medical services and reputation management, including digital reputation management.
In this way, relationship management is a key strategy in building lasting loyalty among consumers of medical services. It should focus on justifying pricing policies, reputation management, and high-quality communications (support, compliance with reviews, etc.).
The CRM paradigm is a tool for building long-term relationships between patients and clinics. In managing patients’ willingness to choose a clinic again, it is a logical addition, as it allows telemedicine, mobile applications, and chatbots to be integrated into a single ecosystem, where the key factors of loyalty are convenience, timely communication, and individual support [10, 24, 25].
This way, digital services not only broaden access to healthcare but also build an emotional and rational connection between patients and clinics, which makes them more likely to come back.
This study provides grounds for outlining a vision for the development of medical tourism based on digitalization and AI integration, particularly in communication processes.
The theoretical basis for the assertion that Ukrainian patients see significant potential for the development of digital medical tourism based on international practices—primarily in the rehabilitation and inclusion segments—is outlined in the approaches Digital Transformation in Medical Tourism [4, 7, 8] and Inclusive Digital Healthcare Framework [21, 23, 26–28]. In particular, the author [27] emphasize the need for parallel implementation of digital innovations in healthcare and improvement of service processes, since it is this interaction that allows increasing the level of inclusiveness, reducing barriers to access, and ensuring wider coverage of patients with medical services.
With regard to empirical arguments, we will first analyze the vision of healthcare consumers in terms of the prospects for the development of medical tourism in Ukraine. Before the war, the potential of the Ukrainian healthcare market was rated quite highly in terms of “price-quality” ratio [29, 30].
Therefore, let us analyze the feasibility of digital medical services in accordance with consumer demand (Figure 11).
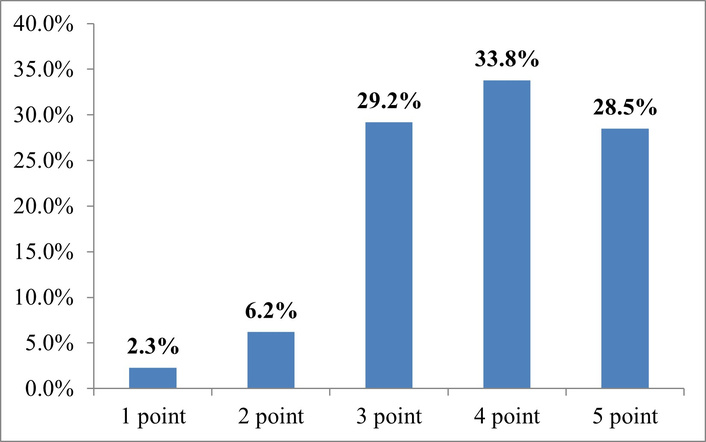
Interpretation of answers to the question “How important is access to digital rehabilitation services (online physiotherapy, psychological support, etc.) to you?”. Source: compiled from anonymized survey results.
The obtained data shows a clear trend towards an increase in demand for remote rehabilitation among Ukrainian patients. A total of 62.3% respondents (rated as “4”—33.8% and “5”—28.5%) consider access to digital rehabilitation to be highly important. At the same time, only 8.5% of respondents (rated “1” and “2”) consider such services to be insignificant.
A substantial proportion of respondents (29.2%) chose the average rating (“3 points”), which may indicate two parallel effects: either insufficient awareness of the possibilities of modern digital rehabilitation (telephysiotherapy, digital progress monitoring, online consultations with a psychologist), or unequal access to such solutions in the regions.
Overall, these results reflect the post-war socio-medical context in Ukraine, where a significant number of patients require long-term rehabilitation after injuries, operations, or psychological consequences of war. Therefore, digital rehabilitation services are becoming not just an additional element of treatment, but also continuously increasing the mobility, accessibility, and inclusiveness of medical care.
This empirically confirms our theoretical assumption that digital rehabilitation is the segment where Ukrainian patients most expect the integration of international practices and innovative solutions.
Given the high level of importance of digital rehabilitation solutions for most respondents, the logical next step was to clarify which formats of digital rehabilitation patients consider most useful and effective in their digital patient journey (Figure 12).
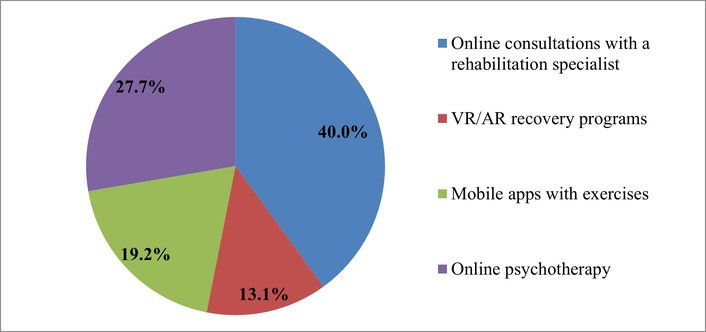
Interpretation of answers to the question “What types of digital rehabilitation do you find most useful?” Source: compiled from anonymized survey results.
The data obtained shows that patients demonstrate differentiated demand for digital rehabilitation services. The greatest interest is focused on online consultations with rehabilitation specialists (40.0%), which indicates the high value of personalized expert interaction. It is important for patients not only to receive information or exercises, but also to have access to professional support in real time. This is consistent with the trend toward hybrid care models, where digital services complement offline visits.
The second most popular area is online psychotherapy (27.7%), which highlights the growing role of psycho-emotional support in the rehabilitation process. This result shows that patients view rehabilitation as a comprehensive process, including the restoration of emotional stability and the reduction of stress levels.
Mobile apps with exercises (19.2%) and VR/AR technologies (13.1%) receiving lower scores, which may be due to both the lower level of digital maturity of patients and the lower availability of relevant technologies. At the same time, these tools have growth potential because they provide autonomy, interactivity, and the possibility of adaptive training.
Overall, the structure of the responses shows that patients prefer digital tools that provide quick access to specialists and increase their subjective sense of security and support. This underscores the importance of developing services focused on personalization, psychological comfort, and multi-channel interaction.
The next step was to determine which digital solutions, according to respondents, are most critical for the development of inclusive medicine in Ukraine (Figure 13).
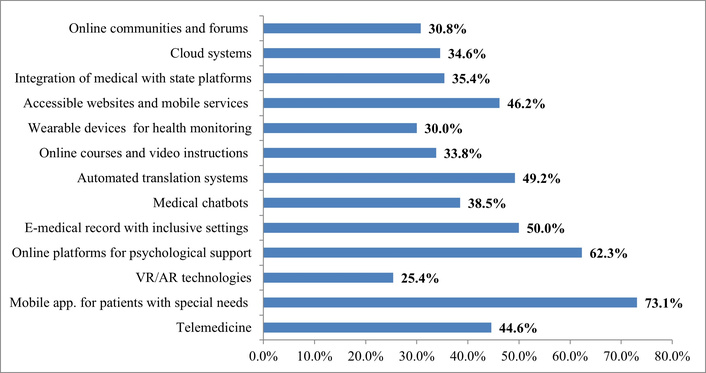
Interpretation of answers to the question “What digital solutions do you consider the most important for the development of inclusive medicine in Ukraine? (Multiple answers are possible)”. Source: compiled from anonymized survey results.
The results show that patients highly value digital solutions that directly enhance the accessibility, personalization, and continuity of healthcare. The most in-demand solutions were mobile applications (e.g., medication reminders, exercises, condition monitoring) for people with special needs (73.1%) and online psychological support platforms (individual and group sessions) (62.3%), highlighting the growing need for daily support, self-directed rehabilitation, and access to mental health. Respondents also noted the importance of electronic medical records with inclusive settings (e.g., easy access for patients with visual/hearing impairments) (50.0%) and accessible websites and mobile services (adapted for people with visual, hearing, motor impairments) (46.2%), online communities and forums for people with disabilities and their families (30.8%) indicating the critical role of digital inclusivity in basic medical infrastructure. Telemedicine (online consultations with doctors and rehabilitation specialists) (44.6%), automated translation systems (text, voice, sign language) (49.2%) and medical chatbots with adapted functions for people with disabilities (38.5%), online courses and video instructions on recovery for patients and caregivers (33.8%) remain significant, providing quick access to information and doctors, especially for people with hearing, vision or mobility impairments. Innovative technologies such as VR/AR technologies for physical and psychological rehabilitation (25.4%) and wearable devices (smart bracelets, sensors) for health monitoring (30.0%), although demonstrating lower levels of support, are still perceived as promising additions to physical and psychological recovery. The focus on data sharing and the digital ecosystem is reflected in the importance of integrating medical and government platforms (e.g., Ukrainian portal of state services “DIIA”) (35.4%) and cloud systems for storing and exchanging medical data between doctors and patients (34.6%).
Overall, the results indicate that patients expect not only technological innovations from the digital healthcare system but also a high level of inclusiveness, convenience, and support throughout the entire treatment and rehabilitation process.
The responses to the open-ended question “Your suggestions or expectations regarding the development of digital services in medical tourism” provided a deeper understanding of consumers’ real expectations regarding the development of digital services in the field of medical tourism. Unlike closed-ended questions, this format revealed a wider range of individual needs, emotional responses, and practical requests from users. Respondents focused on both basic aspects of convenience and accessibility, as well as more innovative solutions involving AI, VR technologies, integration platforms, and personalized digital support. A summary of the comments allowed us to identify key groups of expectations, which are presented below in a structured form (Table 7).
Summary of open responses from respondents (healthcare consumers) regarding the development of digital services in medical tourism.
| Category of suggestions/expectations | Essence of repeated responses | % of similar responses |
|---|---|---|
| A single online platform for medical tourism (directory of clinics, doctors, ratings, booking) | The desire to see a single service for choosing clinics, comparing prices, making appointments, reading reviews, and viewing treatment packages | 42.0% |
| Online medical record/medical passport | Access to test results, medical history, translations into foreign languages, and data exchange between doctors and countries | 36.0% |
| Telemedicine and remote consultations | Online consultations before/after treatment, remote monitoring, and psychological support | 33.0% |
| Convenience, simplicity, and accessibility of digital services | Simple interface, stable operation, ease of use, minimal stress, accessibility for older people | 30.0% |
| Inclusive digital solutions for people with disabilities | Adapted interface, sign language translation, assistive technologies, accessibility | 24.0% |
Source: developed by the authors.
Analysis of respondents’ answers allows us to synthesize the following conclusions:
The strongest demand is for a unified “all-in-one” digital ecosystem that combines search, booking, consultation, test, and support;
There is a very high demand for inclusivity and accessibility, which echoes the results of previous questions;
A significant part of the demand is for transparency and trust, which indicates distrust of current platforms with fake reviews;
Patients want AI-based personalization, but not as a primary function, rather as an extension of basic services;
There is a noticeable desire to simplify the entire patient journey, including logistics, payments, insurance, and translation.
These conclusions form the prerequisites for creating a model of the expected digital service of an “ideal medical tourism platform” that will facilitate the patient’s digital journey (Figure 14).
Four fundamental approaches are used in developing an integrated model of digital interaction with patients, each of which defines a separate dimension of service quality and accessibility. First, the SERVQUAL model provides a framework for assessing the quality of digital medical services through the ratio of expected and actual service. In the context of digital medicine, this means that the main task is to reduce the “quality gap” by combining the personalization of digital solutions and the standardization of key service stages. This ensures service stability while maintaining an individual approach to each patient.
Second, the CRM approach ensures consistency in developing long-term relationships with patients. Its value lies in shifting the focus from one-time medical services to “long-term follow-up”—the patient’s digital journey, which includes communication, reminders, support, post-treatment monitoring, and feedback. This creates a connection that increases trust, loyalty, and the likelihood of choosing the clinic again. Third, the Inclusive Design Framework requires the digital platform to be accessible and universal. This is critically important in the context of medical services, as patients may have different types of limitations: mobility, sensory, cognitive, or related to war-related stress and trauma. Building a service based on the principle of inclusive design means that the platform anticipates various usage scenarios from the outset and does not exclude any user groups. Fourth, the concept of AI-driven care views AI as a tool for optimization, not replacement, of healthcare professionals. Algorithms can speed up pre-triage, analyze symptoms, improve patient routing, and increase the accuracy of personalized recommendations. In this way, AI creates conditions for a faster, safer, and more individualized patient journey.
Together, these approaches form a model of digital medical interaction in which service quality, long-term relationships, inclusiveness, and technological intelligence work as a single system.
Digital medical tourism, as a direction of professional medical care using digital technologies and platforms, is a relevant topic of research today. After all, the provision of some services can be optimized over time and at a distance (between regions, countries), while simplifying processes such as consultation, diagnosis, and post-hospital support. Digitalization is fundamentally changing the behavior and expectations of patients, changing the ways people interact with medical institutions and their staff through online consultations, medical portals, mobile applications, telemedicine and other digital tools. These innovations also simplify access to information about relevant specialists, diagnostic and treatment options, as well as medical institutions, increasing transparency and enabling patients to make informed decisions. The study confirms that a conceptual model of the digital patient journey, including information and navigation, digital diagnostics, travel support, rehabilitation and monitoring, and loyalty and trust, can help engage patients from initial information search to post-hospital support, optimize personalization, and improve multi-channel interactions.
Furthermore, digital services not only expand access but also promote both emotional and rational attachment to clinics, increasing the likelihood of repeat visits. The results highlight the importance of inclusive digital health services, demonstrating high interest among patients with special needs, including online psychological support and rehabilitation consultations. By integrating service quality, long-term relationships, inclusivity, and technological intelligence, the digital patient journey model takes into account critical factors related to healthcare professionals and the medical tourism market, including the international context.
However, each country has its own cultural and national characteristics, so the task of medical tourism is to help the patient navigate the digital journey with the greatest efficiency. The aim of the study was to analyze the experience of a patient in the digital journey in Ukraine, which is experiencing large-scale military challenges. Particular attention was paid to how digital tools can ensure continuity of medical care, increase patient trust, and contribute to the competitiveness of medical institutions. It should be noted that the study has several limitations, which are associated with the multidisciplinary nature of the topic and objective factors. First, the sample size was relatively small (150 respondents, mostly women), and the survey was conducted using an anonymous Google Form questionnaire, which may limit the generalizability of the results. The work does not emphasize the predicate of place of residence (city or village), because in general, Ukrainians have sufficient digital literacy and fluency in digital tools. Also, no forecasts are made regarding the development of medical tourism in Ukraine. There is no such large-scale experience in the world as the war in Ukraine. The scale of deaths and injuries among the military and civilian population is difficult to predict, and daily shelling creates constant threats to the functioning of the medical system. Neither a single person nor any modern AI system can reliably predict either the end date of the war or the long-term consequences for health care. Therefore, within the framework of this study, we state the existence of this problem and propose to consider it as an important direction for future research that requires a separate in-depth analysis. Third, the development of the medical tourism sector in Ukraine is largely shaped by private clinics and volunteer initiatives, with limited participation of state instruments. Therefore, aspects of state influence were also beyond the scope of this study. Finally, the study also did not sufficiently cover digital communication platforms. Messengers and social networks were considered as communication channels, but their broader role in shaping patient perceptions was not explored, which requires further research. Thus, the scientific multi-vector nature of medical tourism and the unprecedented military context in Ukraine create additional difficulties in generalizing the results. Therefore, the study has many directions of scientific development and research topics. Therefore, the inclusion of a wider range of countries and culturally diverse patient groups in future studies will allow for a more comprehensive assessment of how cultural values, patient expectations, and local healthcare practices affect the effectiveness and acceptability of digital tools. Similarly, in the post-war period, it is important to explore new digital interactions and corrections of the patient’s digital journey. As well as Ukraine’s medical potential in the development of digital and physical medicine, the formation of inclusive digital relationships, etc.
Therefore, future research will go beyond these limitations and will be implemented in future works. Primarily, it should aim to validate the digital patient journey model, as well as explore the sustainability, scalability, socio-cultural, and political implications of digital health services. By addressing these areas, future works can further enhance the global relevance of digital patient journey models and help develop strategies for the development of patient-centered digital health services and medical tourism.
CRM: Customer Relationship Management
SDG: Sustainable Development Goals
WHO: World Health Organization
The supplementary material for this article is available at: https://www.explorationpub.com/uploads/Article/file/101189_sup_1.pdf.
LB: Conceptualization, Investigation, Writing—original draft, Writing—review & editing. IM: Conceptualization, Investigation, Writing—original draft, Writing—review & editing. AR: Validation, Writing—review & editing, Supervision. All authors read and approved the submitted version.
The authors declare that they have no conflicts of interest.
The study involved an anonymous patient survey and semi-structured expert interviews focusing on the digital patient journey. No personal identifiers or sensitive medical data were collected, and participation posed no risk to participants.
In accordance with national regulations and institutional guidelines, formal ethical approval from an ethics committee or institutional review board was not required, as the study was based on voluntary, anonymous participation and did not involve any medical intervention or collection of identifiable data.
The research was conducted in full compliance with the ethical principles of the World Medical Association Declaration of Helsinki (2013), including respect for participants, voluntariness, confidentiality, and protection of personal information.
All participants provided informed consent prior to participation in the study. For patients, informed consent was obtained electronically before completing the questionnaire. For expert participants, informed consent was obtained prior to the interviews. Participation was voluntary, and participants were informed about the purpose of the study, the anonymous nature of data collection, and their right to withdraw at any time without consequences.
Not applicable.
The datasets generated and analyzed during the current study are not publicly available due to confidentiality and anonymity assurances given to participants. Aggregated anonymized survey data on digital services in medical tourism, collected via Google Forms, are available from the corresponding author upon reasonable request.
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
© The Author(s) 2026.
Open Exploration maintains a neutral stance on jurisdictional claims in published institutional affiliations and maps. All opinions expressed in this article are the personal views of the author(s) and do not represent the stance of the editorial team or the publisher.
Copyright: © The Author(s) 2026. This is an Open Access article licensed under a Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, sharing, adaptation, distribution and reproduction in any medium or format, for any purpose, even commercially, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
View: 1951
Download: 118
Times Cited: 0
